
Nutrition refers to the process of taking in food and fluids to provide the body with energy, support growth, and repair and maintain overall health. Nutriton provides the raw materials mitochondria need to produce energy.
When we eat carbohydrates, they are broken down by digestive enzymes into glucose, fats are broken down by bile from the liver and digestive enzymes into fatty acids, and the protein we eat are broken down by digestive enzymes into amino acids.
Glucose, fatty acids and amino acids (smaller building blocks) are absorbed into the bloodstream and then taken up by muscle, brain and nerve, heart, and liver cells among others.
Inside the cells, mitochondria act as energy factories, using these fuel sources to produce ATP (adenosine triphosphate), the body’s main source of energy.
Energy problems can arise for a number of reasons in mitochondrial disease. Some disorders affect different energy-producing pathways, depending on the underlying genetic cause. Some individuals have difficulty using carbohydrates efficiently, others may struggle to use fats for energy, and some may be affected by multiple pathways.
Understanding which energy pathways are impacted can help explain why certain nutrition strategies are recommended for specific mitochondrial disorders.
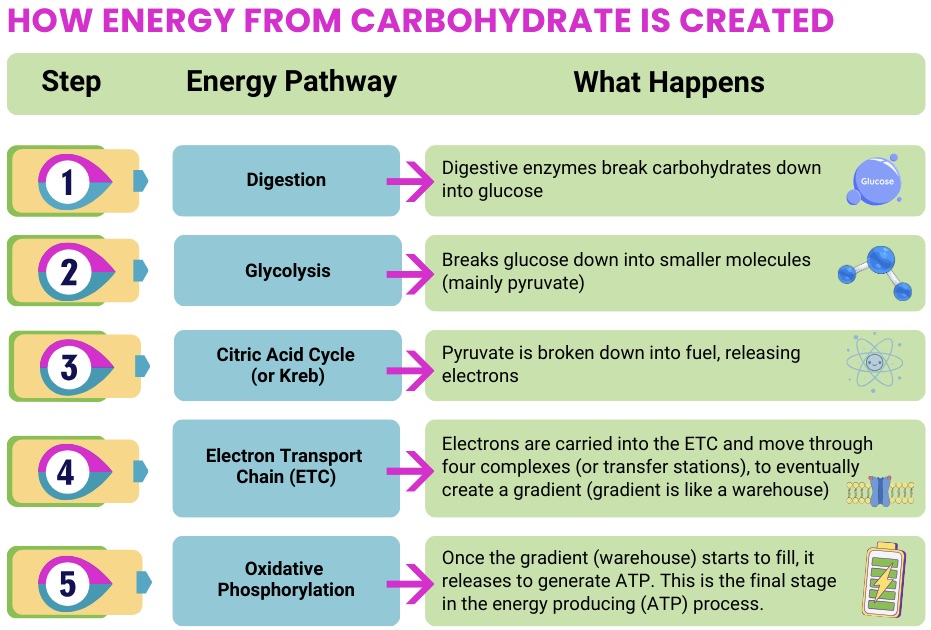
Carbohydrate-Based Energy Pathways
What happens: Glucose is processed and ultimately used by mitochondria to create ATP
When this pathway is impaired:
- The body has difficulty using glucose efficiently for energy, which can lead to energy drops and make the body more reliant on other energy pathways to produce energy.
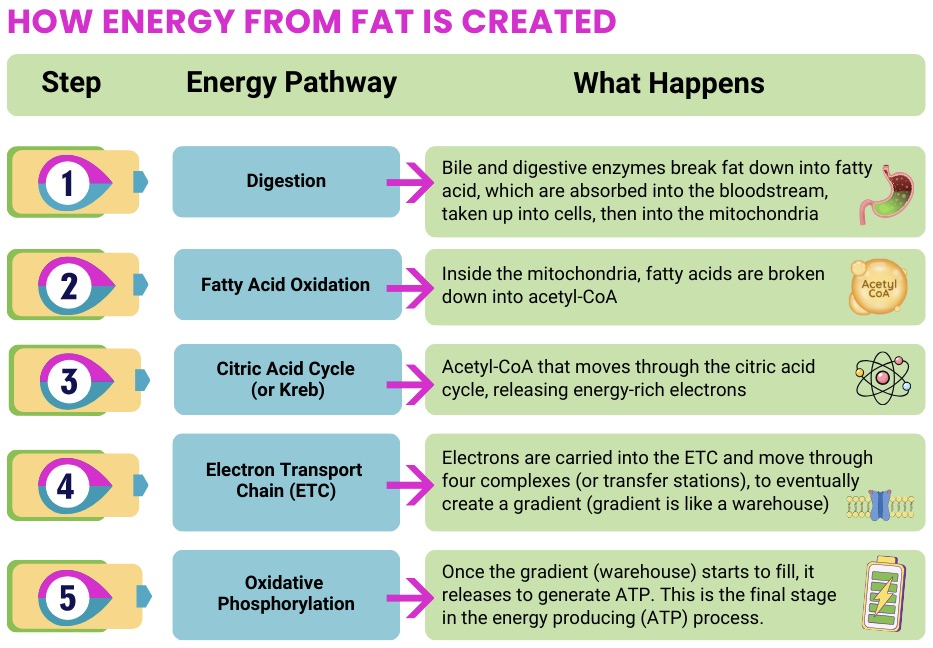
Fat-Based Energy Pathways
What happens: Fatty acids are transported into mitochondria and broken down to create ATP
When this pathway is impaired:
- There’s difficulty using fatty acids as a fuel source, which increases reliance on carbohydrates as a backup. During times illness, fasting or missed meals, the body is more likely to run out of usable energy.
* Oxidative Phosphorylation is the pathway impaired in fatty acid oxidation disorders (FAOD)
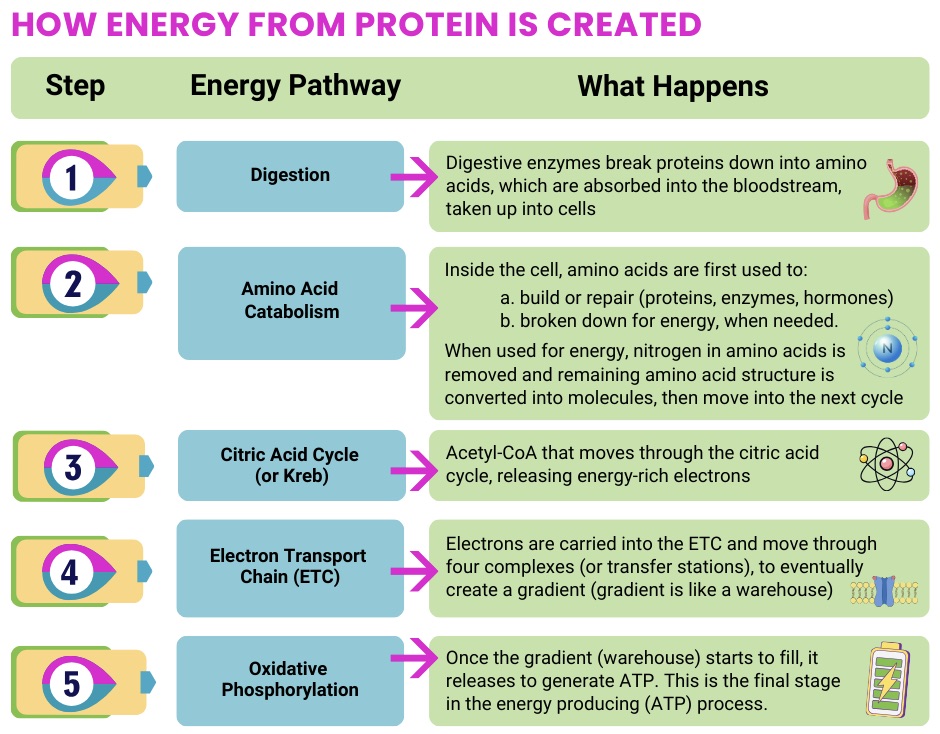
Protein-Based Energy Pathways
What happens: Some amino acids can be used to support energy production, when needed
When this pathway is impaired:
- The body has more difficulty using amino acids for backup energy, which can increase fatigue and place extra strain or workload on other energy systems to compensate.
* Protein (amino acid) is not the body’s preferred fuel source because it’s more complex to breakdown, creating more metabolic stress or making cells in the body work harder to create needed energy.
In mitochondrial disease, any of the above energy-producing pathways may be inefficient or impaired. As a result, individuals may experience fatigue, muscle weakness, exercise intolerance, gastrointestinal symptoms, and difficulties maintaining weight or energy balance.
Thoughtful nutrition strategies can help:
- Support more stable energy production
- Reduce metabolic stress
- Prevent nutrient deficiencies
- Manage symptoms such as fatigue, nausea, and muscle pain
While nutrition is not a cure for mitochondrial disease, it can be a key component of comprehensive care.
